
Hospital and rehabilitation
Your child in hospital after an acquired brain injury, the tests and treatments you may encounter, and the professionals you may meet along the way.
Many diseases can mimic encephalitis, making it hard to diagnose. Mum Sophie explains what this meant for her three-year-old daughter and shares Blair’s progress at The Children’s Trust and back home.

Published: May 2021. Date of brain injury: October 2018 (aged 3 years)
In October 2018, Blair had a focal seizure out of nowhere while playing at her friend’s house. She became absent so her dad Kyle rang for an ambulance.
Blair was given rescue medication and was back to her normal chatty self once coming round in hospital. We were discharged the next day with a possible diagnosis of epilepsy.
After a few days we were all at home and Blair started becoming a little vacant and sleepy yet again and began presenting with some strange behaviours like repetitive blinking so we took her straight to A&E. There they gave her treatments for possible infections and ran all possible tests during our three-day stay, during which Blair became worse and worse and by day three she was hallucinating, screaming (no longer able to talk, walk, eat or even sleep).

At this point we were transferred to the Great North Children's Hospital in Newcastle, still clueless to what was going on and what was wrong with Blair.
Blair was treated straight away for seizures and sedated; she was also given a feeding tube. We met a neurologist who speculated it could be autoimmune encephalitis but that the test would take up to three weeks to confirm it.
When we were transferred onto the Neuro ward in Newcastle we were so happy and relieved Blair was finally being treated by specialist consultants that immediately seemed to know what they were dealing with, especially after three days of complete panic at the previous hospital.
At this point we were still naive to the world of neurology and acquired brain injury – we were hoping they would find out what was wrong, treat it and we would be on our way in a few weeks.
Blair received IVIG, steroids and plasmathesis in the first few weeks. However, she continued to deteriorate and acquired an extreme movement disorder that had her thrashing around the bed whenever she was awake and barely sleeping because of it – no sedatives or sleeping aids seemed to help her rest.
With every new medicine we always had hope that this would be the one to essentially make her better. The doctors would keep saying she needs time – we never ever imagined how much time they were referring to. After the plasmathesis (which did not work either), Blair’s central line became infected and she contracted sepsis. This delayed her next treatment which we were told was the treatment that normally works in autoimmune encephalitis but is somewhat of a last resort due to it's possible side effects. So we just had to wait until Blair fought sepsis off (which was scary in itself) before starting this second line of treatment.
Around this time we received Blair’s diagnosis of NMDA and Anti-GAD Encephalitis (from her spinal tap that was sent to Oxford). We relentlessly searched the internet for similar cases and success stories, we still felt very determined to get her back and of course still had hope; we would never accept Blair could not recover and return in full.

Blair completed her course of Rituximab, which was one dose every week for four weeks. After every treatment we counted down the days for the next hoping that it would work each time, but unfortunately nothing did; we were all still living in hell and were extremely heartbroken after nearly three months of seeing our daughter in such a dreadful way.
The hardest part was hearing that the consultant had never seen this condition in a child so young and so severely ill; there was no experience to go by so everything was new to all involved.
We definitely felt grief, because we had lost our daughter for so long not knowing the outcome. We were never given any hope, just that there was no way of knowing how she would recover if she did.
During Christmas 2018, Rituximab had not worked so we decided to move onto the next line of treatment, cyclophosphamide – a low dose chemotherapy drug.
At this point we would have tried absolutely anything; anything was better than seeing Blair so dreadfully ill and agitated – we were still all in a living hell and so heartbroken. How could a three-year-old go through such unimaginable pain and suffering with no end.
Thankfully after around three rounds of cyclophosphamide in February/March, Blair started tracking with her eyes and holding her head up, and later sitting with aid. She continued to improve physically with daily physiotherapy but after the fourth dose her neutrophils did not return so it was too dangerous to administer any more.
The consultants decided that the amount of cyclophosphamide Blair had received was enough and had done its job, and so we had to push her both physically and cognitively for what would be the next two years in order for her to relearn everything.
We were both very determined to get her back to all her lovely glory, chatting and playing like a normal young girl. Luckily a speech therapist in the Royal Victoria Infirmary told us about The Children's Trust as she had previously worked there; she completed our application and we gratefully accepted a four-month placement there.
I think that if the doctors had been able to give us more knowledge on her condition, and some past stories of other children that had NMDA Encephalitis and recovered, that would have given us the hope we so desperately looked for.
Once we were aware of The Children's Trust we found the real stories very encouraging and I read them all to gain some glimmer of hope. By the time we found it, we had already been through about six months of being in the dark, thinking we were the only people in the world to have had to experience such a dark and devastating illness.
I would have also liked the doctors to give us more hope – but I understand that they could not promise anything due to the nature of brain injury.
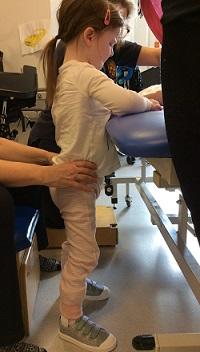
We arrived at The Children's Trust about eight months after Blair became poorly. She was able to stand, aided. She could not talk, eat or walk. We were so desperate to give her as much rehabilitation as was humanly possible and that is what we received at The Children's Trust.
Having full days of rehab was amazing. Unfortunately Blair was still quite heavily sedated due to her movement disorder so missed quite a bit to start with but it was quite flexible. After only three weeks, Blair took her first bite of a crisp, which was the most amazing day ever! It was a weekend and we went to a beautiful park nearby – she was sat on a picnic blanket and started eating.
Blair had an amazing physiotherapist Rachel who we all absolutely loved; she catered all of her classes to suit Blair, like little treasure hunts to get her moving. We took her to the resident soft play every evening and local parks when the weather allowed. We really felt that the four months we were at The Children’s Trust fast tracked her recovery.
The only thing we did not benefit from was the speech therapy. When we left in October 2019 Blair was still non-verbal; it was frustrating for us and we could see it was for Blair too. Since coming off her sedatives though, we can now look back and see that they were intentionally holding her back in that respect. She is now fully talking and will not stop!

At the start, because the situation was critical and acute for a very long time, there was less focus on brain injury and we focused on the fact Blair was extremely poorly and how could we get her better.
We had a lot of support from our close family, which we could not have survived without. We had a 6-month-old at the time so having parents to look after a baby while we cared for our critically ill child was lifesaving. In the long-run it enabled us to maximise Blair's care and recovery, and we put our everything into it which we feel has enabled her to access the support she needed and recover as quick as possible.
We spoke to a physiologist in hospital early on – but we didn't feel it was something we needed as we were so busy trying to help Blair that we couldn't accept that she would have a brain injury or any deficits as a consequence.
When you are experiencing something like that you kind of feel like no-one could possibly understand other than those experiencing it. We had each other and we both knew how we felt and that pushing through was the only way to keep everything together – the one main and important focus, to bring Blair back.
We didn't speak to our wider family or friends during this time, we were too busy and in a bubble where we felt no one could understand what was happening. We knew they would be there when we needed them and that's all that matters at the end of the day.
Blair started talking 18 months after the onset of her illness. At the start of lockdown she could only say ‘yeh’ and ‘na’, and by the end of the second lockdown in August 2020 Blair was talking in full sentences. She can run, hop, skip, jump and do anything she puts her mind to. She started Reception at school, as we decided to hold her back one school year. She has 1:1 support for safety and help if she needs it – but we are hopeful that this is only short-term as Blair is on par with her peers in most ways!
Blair is doing great with her speech but she is still probably a little behind her age. She gets intensive speech therapy at school twice a week and we hope this, along with consistent schooling (once Covid is less of an issue), will bring her back up to the level of her peers.
Physically Blair is great; a little more prone to falls but it is definitely hard to tell with a young child – she has been discharged from physio and occupational therapy (OT). When we arrived at The Children's Trust, Blair could not move her left arm at all, and with daily OT within the first few weeks she was back using her arm. She now has no problems at all with fine motor skills.

Surprisingly, Blair has no problems with fatigue and we haven't noticed any memory issues but she is only five years old so it is again hard to tell. Blair does not remember her ordeal, which we are so pleased about. In hospital we were told that her brain wasn't functioning as she was catatonic and because of this she did not have the capacity to know what was happening to her or even remember it, which I guess gave us some comfort in a way. We do not tailor her day any differently to what we would have, had she not had a brain injury.
We really hope that Blair continues to thrive and we do not encounter any future deficits or learning disabilities due to her illness and subsequent acquired brain injury. We have been told that Blair could encounter some learning difficulties as she moves up in school, but as always neuro consultants err on the side of caution, we are hopeful that she will not.
We always knew that Blair may develop Type 1 Diabetes as a result of her Anti-GAD antibody. She tested positive for COVID in early Spring 2021 and we are unsure but this may have triggered her to become diabetic sooner rather than later. She is now on insulin but has taken it in her stride as she always does. She has had three-weekly IVIG infusions for the past nine months because she is now immunodeficient as a result of her heavy immunosuppressant treatment in hospital. Other than this she is happy and healthy and constantly thriving!
If I was speaking to someone in the same position I would say never give up and always push for what you believe in. Never look back and regret not asking that doctor a silly question or second guessing any advice given. Look for families in similar circumstances and gain comfort from knowing you're not the only one.

Your child in hospital after an acquired brain injury, the tests and treatments you may encounter, and the professionals you may meet along the way.

Frequent seizures led to a diagnosis of autoimmune encephalitis for five-year-old Amelia. Mum Sophie shares their story.

Our series of free books and resources aimed at children and families (P&P costs only).

The Children’s Trust gives children and young people with brain injury and neurodisability the opportunity to live the best life possible by providing specialist rehabilitation, education and community services across the UK.