
Assessments and treatments
Read about the tests and treatments healthcare professionals may carry out after a brain injury.
Mollie was three years old when she became ill. What started as a seemingly nasty virus, quickly turned out to be her parents’ worst nightmare. Mum Ceri shares their story.

Published: July 2020. Date of brain injury: August 2019 (child aged 3 years)
Mollie was admitted to hospital on 13 August and within an hour started to have seizures. It was terrifying to watch our little girl in so much pain, her little body would tense and she would arch her back. It was awful to watch and we felt so helpless.
The team at Worcester hospital were initially perplexed because she didn’t have a temperature and all of her other vitals were seemingly normal. However, when they did several neurological tests they determined that Mollie was very unresponsive and gave her a score of 8/15 on the Glasgow Coma Scale. We later found out that this is classed as severe. She was also fitted with an NG feeding tube as she had lost the ability to eat, drink and swallow. She became incontinent and went back into nappies.
After an EEG test we were told that Mollie’s brainwaves had slowed down and that they were working on a possible diagnosis of encephalitis. They did a lumbar puncture and an MRI scan before confirming the worst possible news. Mollie had sustained devastating swelling to her brain.
They initially gave us a diagnosis of Acute Necrotising Encephalopathy (ANE) and said that she was in a very critical state. They shared the MRI with the neurology team at Birmingham Children’s Hospital who then requested that Mollie be moved there so they could monitor her. She was diagnosed with Acute Disseminated Encephalomyelitis, an autoimmune condition that meant the antibodies in Mollie’s blood were attacking her brain and causing the swelling.
So after five days at Worcester hospital she was transferred to the high dependency unit at Birmingham Children’s Hospital and once settled she had another MRI. Mollie’s neurology team came to see us after the results and told us that they were extremely concerned about her condition and that we needed to prepare ourselves that Mollie might not make it. We were absolutely devastated, how had this happened to our normal, healthy, bouncy little girl.
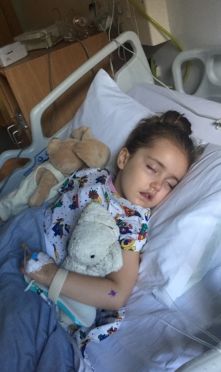
Thankfully Mollie’s condition did begin to improve and after 10 days of being on a combination of antibiotics, antivirals and steroids she woke up. She started to smile and giggle, and we knew we had our little girl back.
Unfortunately, the steroids hadn’t worked as well as the team had expected so they started Mollie on a course of plasma exchanges, which is a bit like dialysis. They put a central line into her femoral artery in her groin and every other day she would be taken to the PICU. They explained to us that Mollie’s blood would be pumped out, put through the filtration system in the machine to filter out her bad plasma and then clean uninfected plasma would be pumped back into her body. The whole process would take four hours, and Mollie had nine of these in total.
Once she was medically stable, that’s when the hard work began as Mollie had to relearn how to hold her head up, sit, roll, crawl, walk, drink and eat again. When we arrived at The Children’s Trust for rehabilitation Mollie had only just started to walk again after being in hospital for eight weeks and home for just four.

She was very wobbly and unsteady on her feet and suffered with fatigue a lot. Relying on her buggy most of the time to get around, Mollie could no longer ride a bike, and found it very difficult to coordinate her movements. She was reliant on me to anticipate all of her needs from food, to dressing, to communicating.
Mollie’s three-month intensive rehabilitation programme included a combination of therapies: physiotherapy, speech and language therapy, occupational therapy, music therapy and hydrotherapy (also known as aquatic therapy), as well as regular psychology and education sessions. It was here that Mollie began to make real progress. She loved her hydro sessions and started to support herself really well in the pool.
A real turning point was about six weeks in when she stopped using her buggy to get around and was able to pedal a pushbike with stabilisers completely on her own.
Today, Mollie is a totally different child to the one that arrived for rehabilitation. She can now walk confidently, even run – which is actually her preferred mode of getting around these days.
Mollie is continuing to make progress now we are home, attending preschool three mornings a week, and is due to start reception in September. Her EHC plan has now been finalised so I’m feeling much more relaxed.
Speech continues to be her biggest challenge due to the verbal dyspraxia she acquired after her brain injury. She does get frustrated, but continues to work hard to communicate with us. She’s does speech and language therapy at home now and we are hopeful that one day she will talk again. She’s also doing ballet and gymnastics classes and I take her swimming once a week, which she loves.
Mollie is continuing to make progress with her speech therapy. We have been very fortunate whilst having to stay at home to receive a daily telephone call from our speech therapist who has been helping Mollie with the sequencing of her sounds. It has made a huge difference and she can now say her name if she breaks it down into two syllables.
We’ve also been keeping busy by doing lots of painting and exploring in the garden.
Whilst Mollie has recovered extremely well, she has been left with acquired verbal dyspraxia, and I have a feeling she will be diagnosed with ADHD soon as well. But I’m just so thankful that she can walk and play with her friends, albeit still being very vulnerable. Mollie’s strength and determination inspires us every day to be better people and will continue to do so. We are hopeful for what her future holds and can’t wait to see what’s next for her.

Read about the tests and treatments healthcare professionals may carry out after a brain injury.

Read our guide to the therapies after brain injury.

Share your family's story. First-hand experiences are invaluable for families caring for a child with a brain injury.